SBRN Celebrates 10 Years!
July 21, 2021
Congratulations to the 2021 SBRN Award Winners!
August 1, 2021Today’s post comes from Dr. Pedro Tauler, Professor of Biochemistry and Molecular Biology in the Department of Fundamental Biology and Health Sciences at the University of the Balearic Islands. In this post, Pedro describes a paper titled “Effects of Habitual Caffeine Intake, Physical Activity Levels, and Sedentary Behavior on the Inflammatory Status in a Healthy Population” that was published in Nutrients. The full-text article is available here (open access). More about the author can be found at the bottom of this post.
Background
Low-grade chronic inflammation is characterized by chronically (two to three-fold) increased concentrations of several cytokines such as interleukin (IL)-6 and tumor necrosis factor (TNF)-α, as well as other pro-inflammatory compounds such as C-reactive protein (CRP). Many chronic diseases such as arthritis or type-2 diabetes, and pathological conditions such as insulin resistance or atherosclerosis have been found to be associated with low-grade systemic inflammation. Sedentary behavior has been linked to low-grade inflammation, independently of physical activity levels or adiposity.
What did we do?
A descriptive cross-sectional study was performed to determine the association between regular caffeine intake, physical activity levels, sedentary behavior and, as the dependent variable, the inflammatory status in a healthy population. Participants in the study were 112 men and 132 women, aged 18 to 55, and belonging to the staff and student population of the University of the Balearic Islands. Plasma concentrations of pro-inflammatory (CRP, TNF-a, IL-6) and anti-inflammatory (IL-10 and adiponectin) markers were measured. Weight, height, and body composition (bioelectrical impedance) as well as diet quality were determined as control variables. Caffeine intake was determined using a food frequency questionnaire focused on foods and beverages containing caffeine. Physical activity levels and sitting time were determined using the International Physical Activity Questionnaire (IPAQ). Therefore, it should be acknowledged that one of the main limitations of the study was that sedentary time was determined using a self-reported questionnaire, and the number, duration, and frequency of sedentary breaks were not recorded. These aspects should be improved in future studies.
What did we find?
Participants in the study (mean age 32.1 years) reported about seven hours of sitting time and moderate physical activity levels. The multivariate regression analysis revealed that sitting time was the main inverse predictor for IL-10 (p<0.001), and a positive predictor for TNF-a (p<0.001). These associations can be observed in Figure 1 (IL-10) and Figure 2 (TNF-a) which shows the cytokine levels in participants stratified per sitting time (tertiles). While associations between pro-inflammatory markers and sedentary behavior have been previously reported, the inverse association between sitting time and IL-10, probably the most important anti-inflammatory cytokine, has not been commonly reported. On the other hand, physical activity was found to be only a weak positive predictor for IL-10 levels (p=0.028).
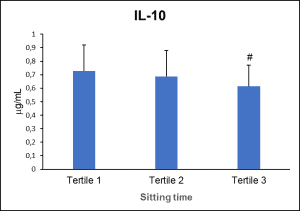
Figure 1. IL-10 plasma concentrations categorized by sitting time tertiles. Means and standard deviations are represented. # indicates significant differences to first tertile.
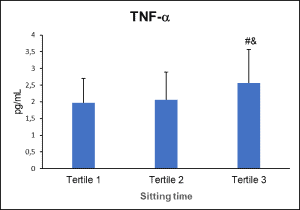
Figure 2. TNF-α plasma concentrations categorized by sitting time tertiles. Means and standard deviations are represented. # indicates significant differences to first tertile. & indicates significant differences to second tertile.
Regarding other results, caffeine intake was a negative predictor of CRP (p=0.001). Body fat percentage was positively associated with CRP (p<0.001) and inversely associated with adiponectin (p=0.032) and IL-10 levels (p=0.001). Visceral fat was the main predictor for IL-6 (p<0.001) and TNF-a (p<0.001).
Conclusions
Sedentary behavior induced pro-inflammatory effects, characterized not only by higher TNF-a levels but by lower IL-10 levels. These results define a pro-inflammatory picture induced by sedentary behavior and independent of physical activity levels. Actually, only slight effects of physical activity levels were observed. It is noteworthy that these results were found in young, healthy and, on average, normal-weight participants. Because it has been reported that active breaks could, to some extent, modify associations between sedentary time and inflammatory markers, at least when sitting time is not too long, policies leading to promote and allow these breaks should be implemented in workplaces such as universities. Despite the current study being limited to data from a single university population, the patterns of sedentary behavior observed could be applied not only to other universities but also to other workplaces with similar characteristics (sedentary patterns of work).
Acknowledgments
This research was funded by the Ministerio de Economía, Industria y Competitividad (MINECO), the Agencia Estatal de Investigación (AEI) and the European Regional Development Funds (ERDF), project DEP2013-45966-P (MINECO/AEI/ERDF, EU).
References
Allison, M. A., Jensky, N. E., Marshall, S. J., Bertoni, A. G., & Cushman, M. (2012). Sedentary behavior and adiposity-associated inflammation: The multi-ethnic study of atherosclerosis. American Journal of Preventive Medicine, 42(1), 8–13. https://doi.org/10.1016/j.amepre.2011.09.023
Gleeson, M., Bishop, N. C., Stensel, D. J., Lindley, M. R., Mastana, S. S., & Nimmo, M. A. (2011). The anti-inflammatory effects of exercise: mechanisms and implications for the prevention and treatment of disease. Nat Rev Immunol, 11(9), 607–615. https://doi.org/nri3041 [pii]10.1038/nri3041
Henson, J., Yates, T., Edwardson, C. L., Khunti, K., Talbot, D., Gray, L. J., Leigh, T. M., Carter, P., & Davies, M. J. (2013). Sedentary time and markers of chronic low-grade inflammation in a high risk population. PLoS ONE, 8(10), 4–9. https://doi.org/10.1371/journal.pone.0078350
Ouchi, N., Parker, J. L., Lugus, J. J., & Walsh, K. (2011). Adipokines in inflammation and metabolic disease. Nature Reviews Immunology, 11(2), 85–97. https://doi.org/10.1038/nri2921
Petersen, A. M. W., & Pedersen, B. K. (2005). The anti-inflammatory effect of exercise. Journal of Applied Physiology, 98(4), 1154–1162. https://doi.org/10.1152/japplphysiol.00164.2004.
Reid, N., Healy, G. N., Gianoudis, J., Formica, M., Gardiner, P. A., Eakin, E. E., Nowson, C. A., & Daly, R. M. (2018). Association of sitting time and breaks in sitting with muscle mass, strength, function, and inflammation in community-dwelling older adults. Osteoporosis International, 29(6), 1341–1350. https://doi.org/10.1007/s00198-018-4428-6
Ross, R. (1999). Atherosclerosis – An inflammatory disease. In New England Journal of Medicine (Vol. 340, Issue 2, pp. 115–126). N Engl J Med. https://doi.org/10.1056/NEJM199901143400207
Yates, T., Khunti, K., Wilmot, E. G., Brady, E., Webb, D., Srinivasan, B., Henson, J., Talbot, D., & Davies, M. J. (2012). Self-reported sitting time and markers of inflammation, insulin resistance, and adiposity. American Journal of Preventive Medicine, 42(1), 1–7. https://doi.org/10.1016/j.amepre.2011.09.022
Citation details
Rodas, L.; Riera-Sampol, A.; Aguilo, A.; Martínez, S.; Tauler, P. Effects of Habitual Caffeine Intake, Physical Activity Levels, and Sedentary Behavior on the Inflammatory Status in a Healthy Population. Nutrients 2020, 12, 2325. https://doi.org/10.3390/nu12082325
About the author

Pedro Tauler is Professor of Biochemistry and Molecular Biology in the Department of Fundamental Biology and Health Sciences at the University of the Balearic Islands (UIB). He is the principal investigator of the group ‘Evidence, Lifestyles and Health” at UIB. He has particular interest in the association between physical activity, sedentary behavior, nutrition and the inflammatory status of the organism. Furthermore, he is interested in the effects of nutrition and supplements, mainly caffeine, on the response to exercise (e.g., inflammatory, immune and oxidative stress). Pedro Tauler has authored about 70 original peer-reviewed articles.